- HAVEN 1 showed emicizumab reduced bleed rate by 87% compared with on-demand bypassing agents
- All 12 secondary endpoints in HAVEN 1 were positive, including an intra-patient comparison that showed emicizumab reduced bleed rate by 79% compared to prior prophylactic bypassing agents
- Data from HAVEN 1 in adults and adolescents and interim data from HAVEN 2 in children with haemophilia A with inhibitors are being presented today at the 26th International Society on Thrombosis and Haemostasis (ISTH) Congress
- Data from both studies have been submitted to FDA and EMA for approval consideration
Roche (SIX: RO, ROG; OTCQX: RHHBY) today announced that data from HAVEN 1, a phase III study evaluating once-weekly subcutaneous emicizumab prophylaxis (preventative) in adults and adolescents with haemophilia A with inhibitors, were published in The New England Journal of Medicine (NEJM). The primary endpoint showed a clinically meaningful and statistically significant reduction in treated bleeds of 87% (risk rate [RR]=0.13, p<0.0001) with emicizumab prophylaxis compared with on-demand (no prophylaxis; episodic use only) bypassing agents (BPAs). All 12 secondary endpoints were positive, including a statistically significant reduction of 79% (RR=0.21, p=0.0003) in treated bleeds in a first of its kind intra-patient analysis in a subset of patients comparing two prophylaxis regimens (emicizumab and BPAs). Data from HAVEN 1 as well as the interim analysis of the phase III HAVEN 2 study of emicizumab in children are being presented at the 26th International Society on Thrombosis and Haemostasis (ISTH) Congress today.
“Nearly one in three people with haemophilia A develop inhibitors to standard factor VIII therapy, leaving them at greater risk of life-threatening bleeds and long-term joint damage,” said Sandra Horning, MD, Roche’s Chief Medical Officer and Head of Global Product Development. “Based on the bleed reduction shown in the HAVEN 1 and HAVEN 2 studies, we believe emicizumab has the potential to make a meaningful difference for people with haemophilia A with inhibitors, while also reducing the burden of managing the condition with a subcutaneous, once-weekly administration.”
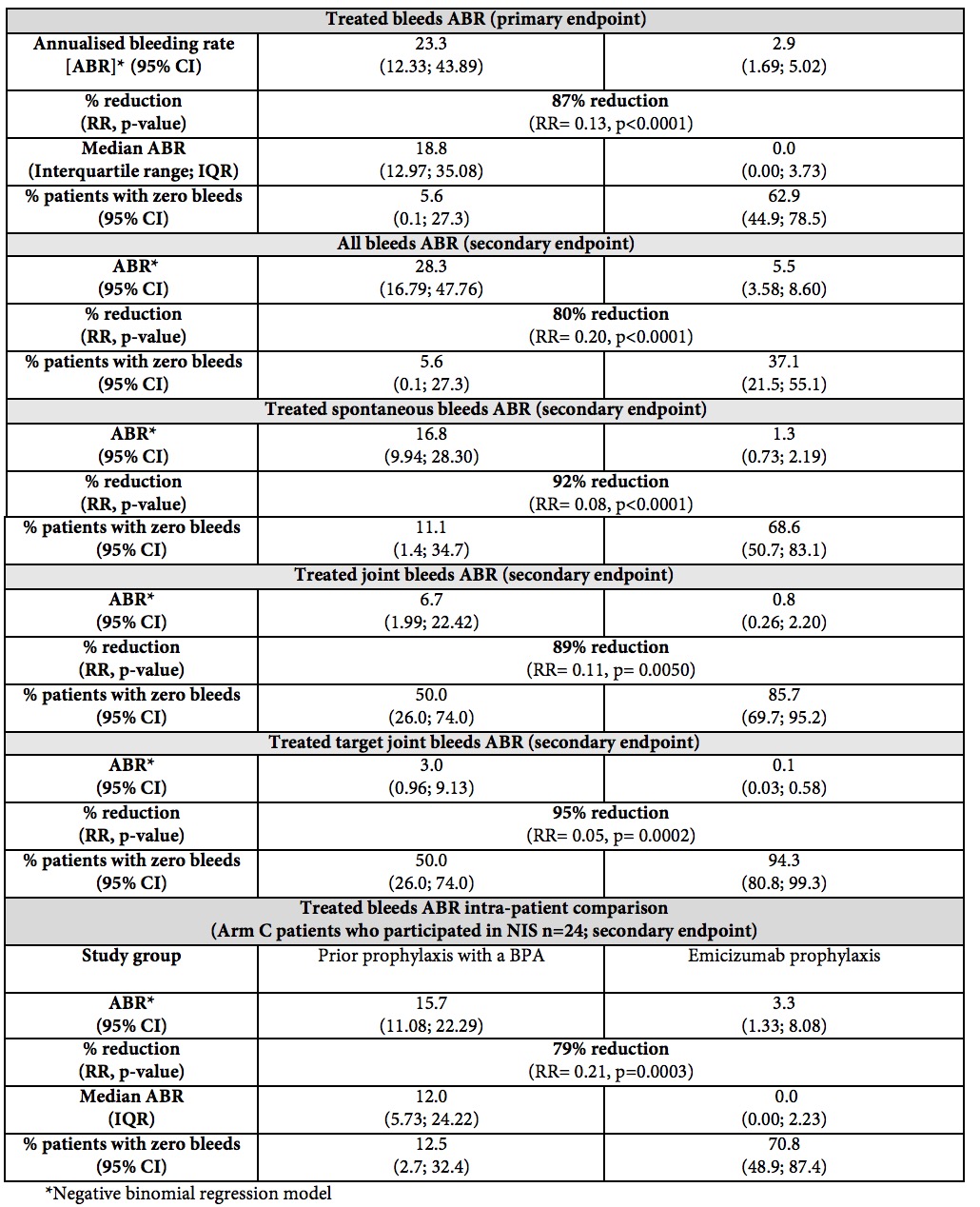
Further data from HAVEN 1 showed that, after a median observation time of 31 weeks, substantially more patients experienced zero bleeds with emicizumab prophylaxis than with on-demand BPAs across all bleed measurements, including zero treated bleeds (62.9% vs 5.6%), zero treated spontaneous bleeds (68.6% vs 11.1%), zero treated joint bleeds (85.7% vs 50.0%), zero treated target joint bleeds (94.3% vs 50.0%) and zero bleeds overall, which includes all treated and non-treated bleeds (37.1% vs 5.6%). A clinically meaningful and statistically significant improvement in health-related quality of life (HRQoL) measured at 25 weeks, using two validated instruments (Haem-A-QoL and EQ-5D-5L), was also observed.
In an additional study arm (Arm C, n=49), patients who had previously received BPA prophylaxis were treated with emicizumab prophylaxis. A subset of patients in this arm (n=24) had previously participated in a non-interventional study (NIS), allowing for a first of its kind intra-patient analysis comparing two prophylaxis regimens. This analysis showed a 79% (RR=0.21, p=0.0003) reduction in treated bleeds in patients receiving emicizumab compared with their prior BPA prophylaxis during the NIS. Data also showed that 70.8% of patients in this subset experienced zero treated bleeds with emicizumab prophylaxis whereas only 12.5% of these patients had experienced zero bleeds with their prior BPA prophylaxis during the NIS.
“The HAVEN 1 study is one of the most robust clinical studies conducted to date in people with haemophilia A with inhibitors to factor VIII, including a first ever intra-patient comparison to prior prophylaxis with bypassing agents,” said Professor Johannes Oldenburg, Institute of Experimental Haematology and Transfusion Medicine, University of Bonn, Germany. “The reduction in bleeding events across all measures seen with emicizumab compared to either on-demand or prophylactic bypassing agents supports that it may be one of the most significant scientific innovations in the treatment of haemophilia A in over 30 years.”
Adverse events (AEs) occurring in 5% or more of patients treated with emicizumab were local injection site reactions, headache, fatigue, upper respiratory tract infection and joint pain (arthralgia). As previously reported, serious adverse events of thromboembolic events (TE) and thrombotic microangiopathy (TMA) occurred in two patients and three patients*, respectively, while receiving emicizumab prophylaxis. The common aspect of these TMA** and TE events is the patients were on emicizumab prophylaxis and received more than 100 u/kg/day of the BPA activated prothrombin complex on average for 24 hours or more before the onset of the event. Neither TE event required anti-coagulation therapy and one patient restarted emicizumab. The cases of TMA observed were transient, and one patient restarted emicizumab.
Interim results from the single arm HAVEN 2 study in children younger than 12 years of age with haemophilia A with inhibitors who received emicizumab prophylaxis are consistent with the positive results from the HAVEN 1 study. After a median observation time of 12 weeks, the study showed that only one of 19 children receiving emicizumab reported a treated bleed. There were no reported joint or muscle bleeds.
An intra-patient comparison (n=8) in a subset of these children who were previously enrolled in the NIS, showed that all experienced a 100% reduction in treated bleeds following treatment with emicizumab (previous annualised bleeding rate [ABR] ranged from 0 to 34.24); this group included seven children who had received prior BPA prophylaxis, and one who had received prior on-demand BPA. The data also indicate that the same dose of emicizumab is appropriate for children as for adults and adolescents, based on the levels of emicizumab in the blood (pharmacokinetics) of the children compared with the levels of emicizumab in the blood of adults and adolescents. The most common AEs with emicizumab in the HAVEN 2 study were mild injection site reactions and common cold symptoms (nasopharyngitis). No TE or TMA events were observed.
“Managing haemophilia A with inhibitors to factor VIII can be especially challenging for children and their caregivers. Not only can bleeding be difficult to control, but current treatments can require frequent intravenous infusions, which can often involve the long-term use of a central venous access device or port,” said Guy Young, MD, Director of Hemostasis and Thrombosis Program, Children’s Hospital Los Angeles, and Professor of Pediatrics, University of Southern California Keck School of Medicine, Los Angeles, California. “The HAVEN 2 interim results indicate that emicizumab may help prevent bleeding in children with inhibitors. Given the once-weekly subcutaneous dosing, it may also help alleviate some of the burden of haemophilia treatment for these children and their parents.”
Data from both HAVEN 1 and HAVEN 2 have been submitted for approval consideration to the European Medicines Agency (EMA) and the US Food and Drug Administration (FDA). The FDA granted Breakthrough Therapy Designation for emicizumab in adults and adolescents with haemophilia A with inhibitors in September 2015. Additional studies evaluating emicizumab in people with haemophilia A both with and without inhibitors and exploring less frequent dosing regimens are ongoing.
About HAVEN 1 (NCT02622321)
HAVEN 1 is a randomised, multicentre, open-label, phase III study evaluating the efficacy, safety, and pharmacokinetics of emicizumab prophylaxis compared to on-demand BPA (no prophylaxis; episodic use only) in adults and adolescents with haemophilia A with inhibitors to factor VIII. The study included 109 patients (12 years of age or older) with haemophilia A with inhibitors to factor VIII, who were previously treated with BPAs on-demand or as prophylaxis. Patients previously treated with on-demand BPAs were randomised in a 2:1 fashion to receive emicizumab prophylaxis (Arm A) or no prophylaxis (Arm B). Patients previously treated with prophylactic BPAs received emicizumab prophylaxis (Arm C). Additional patients previously on BPA (on-demand or prophylaxis) were also enrolled in a separate arm (Arm D). On-demand treatment of breakthrough bleeds with BPAs was allowed per protocol in all arms.
The primary endpoint of the study is the number of treated bleeds over time with emicizumab prophylaxis (Arm A) compared with no prophylaxis (Arm B). Secondary endpoints include all bleed rate, joint bleed rate, spontaneous bleed rate, target joint bleed rate, HRQoL/ health status, intra-patient comparison to bleed rate on their prior prophylaxis regimen with BPAs (Arm C) or no prophylaxis (Arm B). The study also evaluated safety and pharmacokinetics.
A summary of the HAVEN 1 study results to be presented at ISTH is included below.


About HAVEN 2 (NCT02795767)
HAVEN 2 is a single-arm, multicentre, open-label, phase III study evaluating the efficacy, safety, and pharmacokinetics of once-weekly subcutaneous administration of emicizumab. The interim analysis after a median of 12 weeks of treatment included 19 children younger than 12 years of age with haemophilia A with inhibitors to factor VIII, who require treatment with BPAs. The objectives of the study are to evaluate the number of treated bleeds over time with emicizumab prophylaxis, safety, pharmacokinetics, HRQoL and proxy HRQoL with aspects of caregiver burden.
A summary of the HAVEN 2 study interim results presented at ISTH is included below.

About emicizumab (ACE910)
Emicizumab is an investigational bispecific monoclonal antibody designed to bring together factors IXa and X, proteins required to activate the natural coagulation cascade and restore the blood clotting process. Emicizumab can be administered by an injection of a ready-to-use solution under the skin (subcutaneously) once weekly. Emicizumab is being evaluated in pivotal phase III studies in people 12 years of age and older, both with and without inhibitors to factor VIII, and in children under 12 years of age with factor VIII inhibitors. Additional trials are exploring less frequent dosing schedules. The clinical development programme is assessing the safety and efficacy of emicizumab and its potential to help overcome current clinical challenges: the short-lasting effects of existing treatments, the development of factor VIII inhibitors and the need for frequent venous access. Emicizumab was created by Chugai Pharmaceutical Co., Ltd. and is being co-developed by Chugai, Roche and Genentech.
About haemophilia A
Haemophilia A is an inherited, serious disorder in which a person’s blood does not clot properly, leading to uncontrolled and often spontaneous bleeding. Haemophilia A affects around 320,000 people worldwide1,2 approximately 50-60% of whom have a severe form of the disorder.3 People with haemophilia A either lack or do not have enough of a clotting protein called factor VIII. In a healthy person, when a bleed occurs, factor VIII brings together the clotting factors IXa and X, which is a critical step in the formation of a blood clot to help stop bleeding. Depending on the severity of their disorder, people with haemophilia A can bleed frequently, especially into their joints or muscles.1 These bleeds can present a significant health concern as they often cause pain and can lead to chronic swelling, deformity, reduced mobility, and long-term joint damage.4 In addition to impacting a person’s quality of life,5 these bleeds can be life threatening if they go into vital organs, such as the brain.6,7
A serious complication of treatment is the development of inhibitors to factor VIII replacement therapies.8 Inhibitors are antibodies developed by the body’s immune system that bind to and block the efficacy of replacement factor VIII,9 making it difficult, if not impossible to obtain a level of factor VIII sufficient to control bleeding. Most people with haemophilia A who develop inhibitors will infuse BPA therapies, either on-demand (episodic) or as prophylaxis, to control bleeding. This approach is known to be less effective and less predictable than factor VIII replacement therapy in people with haemophilia A without inhibitors.10
About Roche in haematology
For more than 20 years, Roche has been developing medicines that redefine treatment in haematology. Today, we are investing more than ever in our effort to bring innovative treatment options to people with diseases of the blood. In addition to approved medicines MabThera®/Rituxan® (rituximab), Gazyva®/Gazyvaro® (obinutuzumab), and Venclexta™/Venclyxto™ (venetoclax) in collaboration with AbbVie, Roche’s pipeline of investigational haematology medicines includes Tecentriq® (atezolizumab), an anti-CD79b antibody drug conjugate (polatuzumab vedotin/RG7596) and a small molecule antagonist of MDM2 (idasanutlin/RG7388). Roche’s dedication to developing novel molecules in haematology expands beyond malignancy, with the development of the investigational haemophilia A treatment emicizumab (ACE910).
About Roche
Roche is a global pioneer in pharmaceuticals and diagnostics focused on advancing science to improve people’s lives. The combined strengths of pharmaceuticals and diagnostics under one roof have made Roche the leader in personalised healthcare – a strategy that aims to fit the right treatment to each patient in the best way possible.
Roche is the world’s largest biotech company, with truly differentiated medicines in oncology, immunology, infectious diseases, ophthalmology and diseases of the central nervous system. Roche is also the world leader in in vitro diagnostics and tissue-based cancer diagnostics, and a frontrunner in diabetes management.
Founded in 1896, Roche continues to search for better ways to prevent, diagnose and treat diseases and make a sustainable contribution to society. The company also aims to improve patient access to medical innovations by working with all relevant stakeholders. Thirty medicines developed by Roche are included in the World Health Organization Model Lists of Essential Medicines, among them life-saving antibiotics, antimalarials and cancer medicines. Roche has been recognised as the Group Leader in sustainability within the Pharmaceuticals, Biotechnology & Life Sciences Industry eight years in a row by the Dow Jones Sustainability Indices (DJSI).
The Roche Group, headquartered in Basel, Switzerland, is active in over 100 countries and in 2016 employed more than 94,000 people worldwide. In 2016, Roche invested CHF 9.9 billion in R&D and posted sales of CHF 50.6 billion. Genentech, in the United States, is a wholly owned member of the Roche Group. Roche is the majority shareholder in Chugai Pharmaceutical, Japan. For more information, please visit www.roche.com.
All trademarks used or mentioned in this release are protected by law.
References
*One event occurred after the clinical cut-off date for the primary analysis
** Two of these patients had also received recombinant FVIIa (rFVII).
- WFH. Guidelines for the management of hemophilia. 2012. Last accessed July 2017: http://www1.wfh.org/publications/files/pdf-1472.pdf
- Berntorp E, Shapiro AD. Modern haemophilia care. The Lancet 2012; 370:1447-1456.
- Marder VJ, et al. Hemostasis and Thrombosis. Basic Principles and Clinical Practice. 6th Edition, 2013. Milwakee, Wisconsin. Lippincott Williams and Wilkin.
- Franchini M, Mannucci PM. Hemophilia A in the third millennium. Blood Rev 2013; 179-84.
- Flood, E et al. Illustrating the impact of mild/moderate and severe haemophilia on health-related quality of life: hypothesised conceptual models. European Journal of Haematology 2014; 93: Suppl. 75, 9–18.
- Young G. New challenges in hemophilia: long-term outcomes and complications. Hematology Am Soc Hematol Educ Program 2012. 2012; 362–8.
- Zanon E, Iorio A, Rocino A, et al. Intracranial haemorrhage in the Italian population of haemophilia patients with and without inhibitors. Haemophilia 2012; 18: 39–45.
- Gomez K, et al. Key issues in inhibitor management in patients with haemophilia. Blood Transfus. 2014; 12:s319–s329.
- Whelan, SF, et al. Distinct characteristics of antibody responses against factor VIII in healthy individuals and in different cohorts of hemophilia A patients. Blood 2013; 121: 1039-48
- Berntorp E. Differential response to bypassing agents complicates treatment in patients with haemophilia and inhibitors. Haemophilia 2009; 15:3-10.
get the latest news and updates to your inbox.